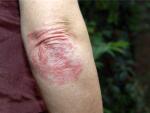
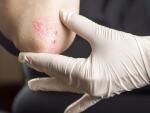
As a doctor who specializes in dermatology, I like to think of the skin as a layer cake. Psoriasis is a disorder of the “icing” on the cake — the top layer of the skin, referred to as the epidermis. With psoriasis, there’s a problem in the immune system that causes your skin cells to replicate too fast. The body becomes a skin-producing machine and can’t slough off or get rid of the new skin cells quickly enough. The result of these changes is the development of red, raised, scaly patches called plaques.
Psoriasis can be a very difficult condition to cope with and manage. Although there is currently no cure for psoriasis, we have made tremendous strides in understanding why psoriasis occurs.This has led to the development of some wonderful new drugs which can manage and improve your skin’s appearance. Here are some important tips for psoriasis patients to consider as they move forward with a treatment plan.
1. Find the right doctor.
Psoriasis patients should first seek out the care of a board-certified dermatologist. A general practitioner might be able to address mild cases of psoriasis, but a dermatologist has the skills and training that you should be looking for. Since psoriasis affects everyone differently, it’s important to connect with a doctor that you can trust and relate to.
For example, when I evaluate psoriasis patients for the first time, I will listen to them to get their story and try to take into account all the factors that might be affecting their psoriasis, including stress, worry, recent illnesses, etc. I will attempt to develop a rapport with my patients by listening to their concerns and struggles and encouraging them to open up. When they show progress, we will share in their joy, and when they regress and are frustrated, I will let them vent and suggest new therapeutic options that might work better. The “right doctor” may not always have the impact you are looking for after the first meeting, but if he or she stays engaged with you, is willing to ride out the ups and downs with you, and is well versed in the latest treatments, then you’re going to have a much better experience and, in many instances, better results.
2. Commit to a treatment plan.
Staying with a treatment plan is important when managing psoriasis. If you can commit to using your medications as directed, keeping your follow-up appointments and maintaining an open line of communication with your dermatologist, you are more likely to have success with treatment. When it comes to psoriasis improvement, I think that a physician contributes 30% and the patient contributes 70% in terms of impact. These numbers illustrate how important it is for patients to commit to a treatment plan. If you stop following your doctor’s advice, there’s a risk the disease will progress and it’ll be harder to manage. If you’re unhappy with your medication, whether it’s due to side effects or other reasons, talk to your doctor about your concerns. Together, you can “reboot” the approach and come up with an alternative plan to effectively treat your psoriasis.
3. Be open to new treatment options.
There are a lot of new therapies out there, so if one treatment isn’t working out, we are fortunate to have plenty of others. For milder cases of psoriasis, medications applied directly to the skin can usually do the trick, but in more severe cases, a new class of drugs called biologics offers great results. Biologics target psoriasis by influencing your immune system and for many patients, they’ve made a huge difference. I’ll often have patients come in for an appointment and ask me about a new psoriasis drug that they are convinced will work for them. I am always impressed with their initiative. Be an advocate for yourself and stay up to date on new treatments. A good resource is the National Psoriasis Foundation.
4. Take care of your mental health, too.
Although psoriasis is a physical disease, it can greatly affect one’s mental health as well. Many of my patients are young adults trying to look their best, and psoriasis can make that difficult. Often they are insecure and afraid to do what most people take for granted, like shake hands or wear short sleeves. Depression and anxiety are common for those with psoriasis. It is important to provide these patients with emotional support and a strong connection with groups or counselors who can encourage them.
As a dermatologist, I advise my psoriasis patients that they are not alone in their struggle. Many times those afflicted feel they’re on an island by themselves, so I encourage them to join support groups and stay connected with other people who are living full and active lives with their psoriasis. There is definitely hope. Keeping balanced mentally can help you to simultaneously clear your skin and stay in control.
5. Lifestyle changes can make a big impact.
Doctors agree that obesity and psoriasis are linked; psoriasis symptoms are often worse in patients who have obesity. This association is really crucial to acknowledge. It’s important to follow a balanced diet and exercise program as well as to minimize the use of tobacco and alcohol.
I want patients to understand that psoriasis can be successfully treated by connecting with the right doctor, committing to a treatment plan, staying educated, prioritizing their mental health, and making smart, healthy lifestyle choices. If patients can do this, they will create the right set of circumstances to manage their psoriasis effectively.